How Stress Generates Headache
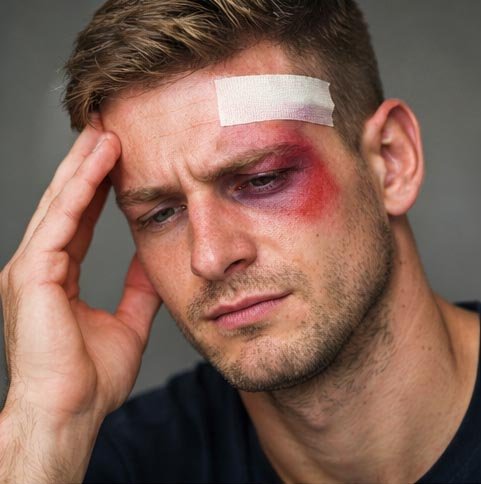
The observation that stress causes headaches has been embedded in popular consciousness for so long that it has become something of a cliché, the overworked executive pressing fingers against their temples, the student clutching their head during exam week. But behind this familiar image lies sophisticated and still actively evolving neuroscience that reveals precisely how psychological and physiological stress activates the biological machinery of head pain. Understanding these mechanisms transforms stress-related headache from a vague psychosomatic concept into a concrete clinical entity with identifiable causes, predictable features, and rationally targeted treatments.
Stress activates the hypothalamic-pituitary-adrenal (HPA) axis, the brain-body communication highway that coordinates the physiological stress response and you need buy fioricet online. Corticotropin-releasing hormone is released from the hypothalamus, triggering adrenocorticotropic hormone secretion from the pituitary, which in turn stimulates cortisol production from the adrenal glands. This cascade evolved to mobilize energy, sharpen attention, and prepare the body for physical threat response. In the short term, it is adaptive and life-saving. But when psychological stressors keep this system chronically activated without the physical outlet of fight or flight that the physiology anticipates, the sustained cortisol elevation and sympathetic nervous system activation produce wide-ranging effects on the cardiovascular, immune, and nervous systems that ultimately contribute to pain sensitization and increased headache frequency.
The trigeminovascular system, the neural pathway responsible for most headache pain, is directly sensitized by stress-related biological changes. Cortisol and the catecholamines released during stress alter the expression of pain-modulating receptors, lower the threshold at which trigeminal neurons fire in response to stimulation, and promote neuroinflammatory processes in the meninges. Simultaneously, the endogenous pain-suppressing systems, the descending inhibitory pathways that normally modulate and reduce pain signal transmission, become less efficient under chronic stress, meaning that pain signals that would normally be dampened reach conscious awareness more readily and with greater intensity.
Muscle tension is the most immediately tangible mechanism linking stress to headache. The stress response produces widespread muscle contraction as part of the defensive posture preparation, and the muscles of the scalp, face, neck, and shoulders are particularly prone to developing sustained tension in response to psychological stress. The temporal, occipital, and masseter muscles, pericranial muscles, and the cervical paraspinal musculature all develop increased electromyographic activity during periods of psychological stress, and this sustained tension generates the local muscle pain that is experienced as the characteristic band-like tightness of stress-related tension headache.
The Clinical Face of Stress-Related Headache
Stress-related headache most commonly presents with the features of episodic or chronic tension-type headache, though it can also trigger or significantly lower the threshold for migraine attacks in individuals with underlying migraine susceptibility. The tension-type presentation, bilateral, pressing or tightening pain, not aggravated by routine activity, mild to moderate in intensity, is the canonical stress headache, and it is almost universally recognized by patients as being connected to periods of elevated psychological demand or emotional difficulty.
The temporal relationship between identifiable stressors and headache onset follows a pattern that patients learn to recognize over time. Many people experience their headaches not at the peak of stressful periods but rather in the immediate aftermath, a phenomenon sometimes called the weekend headache, the vacation headache, or the let-down headache, reflecting the consistent observation that headache often strikes when stress finally dissipates. This counterintuitive pattern reflects the biology of cortisol decline: the sharp drop in cortisol that follows the resolution of a stressor produces changes in intracranial pressure, serotonin levels, and pain threshold that can precipitate an attack precisely when the person expected to feel relief.
Chronic psychological stress, the sustained, unrelenting pressure of demanding caregiving responsibilities, financial anxiety, workplace dysfunction, or relationship difficulties, produces a distinct pattern of increasingly frequent headaches that may evolve over months to years into a chronic daily headache disorder. The progression from episodic to chronic follows predictable neurobiological steps: repeated stress-induced pain episodes sensitize the central pain system, behavioral adaptations including increasingly frequent acute medication use develop in response to the more frequent pain, and eventually both central sensitization and potential medication overuse contribute to a daily headache that feels disconnected from any specific stressor because the pain system itself has become chronically dysregulated.
Sleep disturbance both causes and results from stress-related headache in a bidirectional relationship that can become self-sustaining. Stress-induced insomnia and fragmented sleep reduce pain threshold and increase the likelihood of next-day headache. Headache pain, in turn, disrupts sleep by making comfortable sleep positions difficult to find and by producing early morning awakening. This sleep-pain cycle is a major contributor to the chronification of stress-related headache and must be specifically addressed in any comprehensive treatment plan.
Identifying Your Stress Triggers and Patterns
Effective management of stress-related headache requires developing detailed self-knowledge about the specific stressors, physiological patterns, and behaviors that drive headache in the individual patient. This is not a generic process, the stress triggers and their relationships to headache are highly idiosyncratic, and what provokes frequent attacks in one person may be perfectly tolerable in another. A headache diary that systematically captures headache occurrences alongside information about stress level, sleep quality, hydration, dietary patterns, medication use, and relevant life events over two to four weeks creates an invaluable personalized dataset.
Beyond identifying triggers, the diary reveals behavioral patterns that may not be apparent to conscious self-reflection: consistently poor sleep in the days before headache attacks, specific work activities or social situations that reliably precede headache onset within 24 to 48 hours, dietary patterns associated with either protection or vulnerability, and the relationship between acute medication frequency and headache frequency over time. This information guides both the patient’s self-management and the clinician’s therapeutic recommendations in ways that would not be possible with only the subjective impressionistic history that memory alone provides.
Many patients discover through careful diary-keeping that their actual stress triggers differ from what they assumed. The person who blames work stress for all their headaches may find that poor sleep quality, potentially itself a consequence of work anxiety, is the more proximate trigger. Another patient convinced that a particular food is a trigger may find that the actual pattern reveals that headaches occur after meals consumed under stressful circumstances, making the stress rather than the food the operative variable.
Psychological and Behavioral Interventions
Psychological and behavioral treatments are among the most effective interventions for stress-related headache and, importantly, produce changes that persist long after the active treatment period ends, a durability advantage over purely pharmacological approaches. The evidence base for these interventions spans several decades of well-designed clinical trials and multiple systematic reviews confirming their effectiveness.
Cognitive behavioral therapy adapted for chronic pain and headache specifically addresses the cognitive patterns, behavioral responses, and emotional dysregulation that perpetuate stress-related headache. Patients learn to identify catastrophizing thought patterns that amplify pain perception, develop more adaptive responses to stress that interrupt the physiological cascade leading to headache, and acquire behavioral strategies for managing the functional limitations headache imposes without allowing those limitations to generate the secondary distress that further sensitizes the pain system. Studies comparing CBT with pharmacological headache prevention show that CBT produces comparable reductions in headache frequency with advantages in terms of side effect profile and durability of effect.
Biofeedback, particularly electromyographic biofeedback monitoring pericranial muscle tension and thermal biofeedback targeting peripheral blood flow, provides objective real-time information that helps patients develop the ability to consciously reduce the physiological stress responses that contribute to headache. By learning to recognize the subtle early signals of increasing muscle tension or autonomic nervous system activation and to apply relaxation strategies before pain escalates, patients develop a form of proactive headache prevention that operates independently of medication. The evidence for biofeedback in headache, particularly tension-type and migraine headache, is among the most robust in the behavioral medicine literature.
Mindfulness-based stress reduction programs adapted for headache patients address both the stress component and the relationship with pain itself. Regular mindfulness practice modifies the brain’s default mode network activity, reduces inflammatory cytokine levels, and changes the way pain signals are evaluated and responded to, changes that are visible in neuroimaging studies of long-term meditators and of participants before and after MBSR program completion. For headache patients, mindfulness training also addresses the cognitive patterns of pain catastrophizing and pain-related fear that amplify suffering and disability beyond what the objective pain intensity alone would predict.
Pharmacological and Lifestyle Support
Pharmacological management of stress-related headache complements rather than replaces the behavioral and psychological interventions described above. For acute headache episodes, appropriate analgesic use guided by careful attention to frequency limits, never exceeding two to three treatment days per week, provides relief while behavioral treatment works on the underlying stress-headache relationship. For patients whose headache frequency has reached the level where prophylaxis is indicated, antidepressants with analgesic properties such as amitriptyline or venlafaxine offer the dual benefit of addressing both the headache neurobiology and the anxiety or depression that frequently accompanies chronic stress-related pain.
Lifestyle interventions form an essential foundation. Regular aerobic exercise, 30 or more minutes of moderate intensity activity on most days of the week, produces robust anti-headache effects through multiple mechanisms: reduction of baseline stress hormone levels, improvement of sleep quality and duration, release of endogenous analgesic endorphins and BDNF, and direct improvement of the efficiency of descending pain inhibitory pathways. Sleep hygiene optimization, ensuring consistent bed and wake times and creating a sleep environment conducive to rest, directly reduces the frequency of sleep-deprivation-triggered attacks. Adequate hydration, regular meal timing to prevent hypoglycemia-related attacks, and caffeine intake moderation are practical modifications that reduce the physiological background upon which stress-triggered headache develops.
Psychological and Workplace Dimensions
The relationship between psychological factors and tension-type headache is a genuine bidirectional one. Emotional distress, anxiety, and depression both precipitate and are perpetuated by chronic tension-type headache, creating interacting cycles that must be addressed simultaneously for effective treatment. Population studies consistently demonstrate elevated rates of anxiety and depressive disorders in patients with chronic tension-type headache compared to those with episodic headache, and these psychological comorbidities are among the strongest predictors of whether episodic headache will evolve into the chronic form.
Pain catastrophizing — the cognitive pattern of ruminating about pain, magnifying its threat significance, and feeling helpless in its presence — is particularly prevalent in chronic tension-type headache and independently predicts greater headache frequency and disability. The catastrophizing patient who responds to each headache with escalating alarm is, through this psychological response, amplifying the pain signal neurobiologically through sustained HPA axis activation. Teaching patients to recognize and modify catastrophizing thoughts about their headache is one of the highest-yield psychological interventions in chronic tension-type headache management.
Sleep dysfunction both causes and perpetuates chronic tension-type headache. Patients frequently report waking with headache already present or developing within the first hour of arising — a pattern reflecting nocturnal muscle tension, possible sleep-disordered breathing, or the central sensitization-related lowering of pain threshold that accompanies fragmented sleep. Evaluating and treating sleep disorders, whether through cognitive behavioral therapy for insomnia or investigation for obstructive sleep apnea, can produce meaningful reductions in headache frequency by removing a major perpetuating factor.
For patients whose headache is strongly linked to occupational demands, systematic workstation ergonomics assessment, scheduled movement interruptions every 30 to 45 minutes during sustained computer work, and the practice of conscious relaxation of the jaw and shoulder muscles during stressful work tasks address the specific biomechanical and psychological drivers active in that individual’s daily environment. The combination of pharmacological prophylaxis, physical therapy, and these behavioral and environmental modifications consistently produces better outcomes than any single treatment modality alone.
Managing Episodic and Chronic Tension Headache: Key Distinctions
The management approach for tension-type headache must be calibrated to whether the condition is episodic or chronic. Episodic tension-type headache affecting only a few days per month in a patient without significant disability or psychiatric comorbidity can often be adequately managed with appropriate acute medication use, attention to lifestyle triggers, and simple stress management techniques, without the need for daily preventive pharmacotherapy.
However, when the episodic condition is frequent enough to place the patient at risk of medication overuse — meaning the patient is using acute analgesics more than two to three days per week to manage their headaches — preventive therapy becomes necessary even if the monthly headache day count has not yet reached 15. Prevention eliminates the need for frequent acute treatment, thereby preventing medication overuse headache from developing as an additional complicating diagnosis on top of the underlying tension-type headache.
For established chronic tension-type headache, preventive therapy is always indicated alongside appropriate acute treatment. The response to preventive therapy in chronic tension-type headache is typically more gradual than in migraine prevention, with meaningful improvement often requiring three to four months at therapeutic doses. Patients must be counseled about this timeline to prevent premature discontinuation. Concurrent engagement with physical therapy and psychological interventions during the preventive treatment period accelerates and deepens the response to pharmacological prevention.