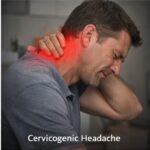
pain originating from structural or functional abnormalities of the cervical spine that is referred to the head through convergent neural pathways shared between cervical and trigeminal afferents — represents one of the most clinically significant and frequently misdiagnosed secondary headache disorders encountered in headache specialty practice. The condition accounts for an estimated four to twenty percent of all chronic headache presentations at specialist clinics, yet the majority of affected patients receive diagnoses of migraine or tension-type headache and treatments appropriate for those primary headache disorders, sometimes for years, before the cervical origin of their pain is recognized. This diagnostic delay has significant consequences: patients accumulate unnecessary pharmacological burden from ineffective headache medications, miss the opportunity for the targeted physical therapy and interventional procedures that would address the actual pain source, and suffer prolonged disability from a condition that responds well to correctly directed treatment.
The debilitating end of the cervicogenic headache spectrum — where pain intensity is severe, functional impairment is marked, and episodes occur with high frequency — requires comprehensive multimodal management that integrates cervical-targeted physical therapy, interventional procedures, and pharmacological support. For patients with severe cervicogenic headache episodes requiring acute analgesic management beyond NSAIDs and simple analgesics, prescription combination analgesics addressing both the pain and the muscular spasm component may be incorporated into a comprehensive treatment plan. Patients seeking buy Fioricet online prescription requirements consultation through licensed telehealth platforms for severe cervicogenic headache should engage with providers who are familiar with the specific clinical features and management principles of cervicogenic headache rather than generalist headache management approaches, ensuring that Fioricet is prescribed within the appropriate context of concurrent cervical-targeted treatment.
Cervical Anatomy and Pain Generation
The anatomical basis of cervicogenic headache lies in the convergence of nociceptive signals from upper cervical structures — particularly the C1 through C3 spinal levels — with nociceptive signals from cranial structures within the trigeminal nucleus caudalis of the caudal brainstem. This convergence means that pain arising from structures innervated by the upper cervical nerve roots is perceived in the same cranial territories as pain from trigeminal structures, producing referred headache that is genuinely experienced in the head despite originating in the neck. The upper cervical facet joints, the atlantooccipital and atlantoaxial joints, the cervical intervertebral discs at the upper levels, and the suboccipital musculature are the structures most commonly implicated in generating cervicogenic headache.
The third occipital nerve, arising from the superficial medial branch of the C3 dorsal ramus and innervating the C2-C3 zygapophyseal joint and overlying skin, is one of the most important single neural structures in cervicogenic headache. Third occipital nerve-mediated pain from C2-C3 facet joint pathology produces referred pain to the occipital and hemicranial regions that closely resembles the distribution of migraine, explaining why cervicogenic headache from this source is so frequently misdiagnosed. Third occipital nerve diagnostic blocks — injection of local anesthetic precisely targeting this nerve under fluoroscopic guidance — both confirm the diagnosis and provide temporary therapeutic relief that predicts response to radiofrequency denervation.
The suboccipital muscles — the rectus capitis posterior major and minor, and the obliquus capitis superior and inferior — are densely innervated muscles that are uniquely vulnerable to both direct injury from whiplash-mechanism trauma and to the chronic overloading imposed by sustained forward head posture. These muscles form myofascial trigger points that generate referred pain to the occiput, vertex, and periorbital region in patterns that are clinically indistinguishable from both tension-type and migraine-type headache, and their contribution to cervicogenic headache is frequently overlooked in clinical assessments that focus on articular rather than myofascial pain generators. The combined articular and myofascial components of cervicogenic headache require both joint-targeted and muscle-targeted treatments for comprehensive management.
Diagnosis and Clinical Assessment
The clinical diagnosis of cervicogenic headache requires a combination of characteristic symptom features and physical examination findings that together distinguish it from primary headache disorders. The headache is typically unilateral without side-shifting, beginning in the occipital or upper cervical region and radiating forward to the temple, forehead, or periorbital area on the ipsilateral side. It is consistently provoked or worsened by specific neck movements or sustained head positions, and physical examination reveals restricted cervical range of motion, tenderness over the upper cervical facet joints, and reproduction of the characteristic headache by sustained manual pressure on specific cervical segments. These examination findings — particularly the reproduction of the patient’s familiar headache by cervical palpation — provide the most diagnostically specific evidence of cervicogenic headache and should be systematically sought in any patient with chronic headache who reports neck pain or cervical stiffness as associated features.
Diagnostic nerve blocks, administered under imaging guidance by trained interventional pain physicians, provide the most definitive confirmation of cervicogenic headache from specific cervical sources. A positive diagnostic block — defined as at least fifty to eighty percent pain relief for a duration consistent with the local anesthetic used — both confirms the cervical origin of the headache and identifies the specific structural level responsible, information essential for planning targeted therapeutic interventions. Comparative blocks using local anesthetics of different durations reduce the false positive rate inherent in single blocks and are required by some guidelines before proceeding to therapeutic interventions such as radiofrequency denervation.
Pharmacological Management
The pharmacological management of debilitating cervicogenic headache addresses acute pain control and, where central sensitization has developed, the prevention of headache chronification. NSAIDs reduce the inflammatory component of cervical joint and soft tissue pain and provide analgesic benefit for mild to moderate episodes. For severe acute episodes that do not respond adequately to NSAIDs or simple analgesics, prescription combination analgesics targeting both the pain and the cervical muscle spasm component are appropriate components of the acute management plan. Patients directed to access buy Fioricet online clinical use information through licensed telehealth services for acute cervicogenic headache rescue should understand that the butalbital component specifically targets the centrally maintained cervical muscle spasm that frequently constitutes the primary pain driver during severe cervicogenic episodes.
Tricyclic antidepressants at low preventive doses — amitriptyline 10 to 25 mg at bedtime — reduce central sensitization in patients with established chronic cervicogenic headache and improve sleep quality, both of which are important for reducing headache frequency and severity over time. The specific cervical pathology driving cervicogenic headache — facet joint arthrosis, disc degeneration, ligamentous injury — benefits from targeted interventional management including cervical facet joint injections and medial branch radiofrequency ablation that pharmacological treatment cannot substitute. The combination of appropriately supervised short-term Fioricet for acute rescue with concurrent cervical-targeted physical therapy and interventional procedures when indicated produces outcomes that substantially exceed what either pharmacological or procedural approaches achieve in isolation. Patients accessing order Fioricet online healthcare consultation services during the acute phase of severe cervicogenic headache should discuss with their provider a plan for transitioning from pharmacological support to the physical and interventional treatments that address the underlying cervical pathology.
Physical Rehabilitation
Physical therapy is the cornerstone of long-term cervicogenic headache management and produces the most durable improvements when targeted precisely at the specific cervical dysfunction driving the headache. High-velocity low-amplitude cervical manipulation and mobilization — when applied by a trained therapist to appropriately screened patients — produces significant reductions in cervicogenic headache frequency and intensity that are superior to medication management alone in multiple randomized controlled trials. Deep cervical flexor retraining, addressing the weakness and inhibition of the longus colli and longus capitis muscles that characterizes cervicogenic headache patients, restores the segmental stability and motor control deficits that perpetuate cervical mechanical overload and headache recurrence. Postural correction exercises addressing the forward head carriage that increases mechanical loading on the upper cervical structures responsible for cervicogenic headache generation provide essential long-term maintenance of the improvements achieved through hands-on physiotherapy. Patients accessing buy Fioricet online prescription service platforms for acute cervicogenic headache management should actively engage with the physical rehabilitation component of their treatment, recognizing that reducing their dependence on acute pharmacological rescue is achievable only through addressing the underlying cervical dysfunction that generates their headaches.